Retinal Detachment in Singapore
All about the retina
The retina is the light-sensitive nerve layer at the back of your eye that sends images to your brain.
Imagine the eye to be like a camera. The retina is the light-sensitive film in the camera in which images are processed. In the human eye, the lens in the front focuses light onto the retina at the back. From there, signals are transmitted to your brain where they are processed, and you interpret these as images.
What is retinal detachment?
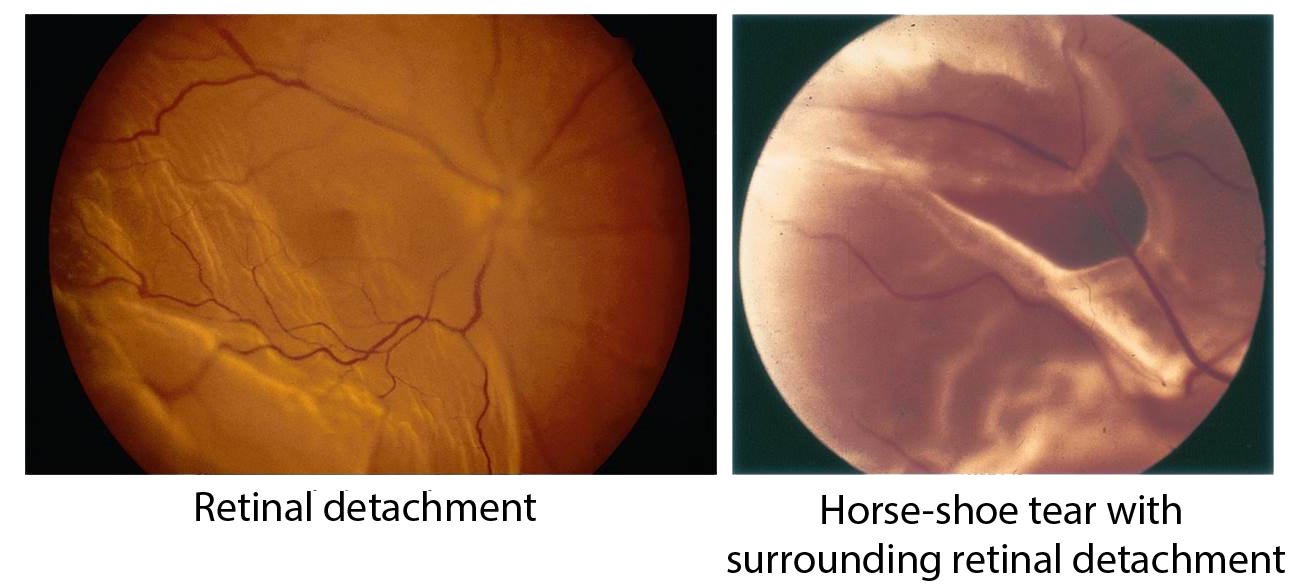
Retinal detachment is a condition whereby the retina is pulled away from its normal position in the wall of the eye. When the retina is detached, it does not function. Your vision is blurred, and blindness almost always ensues unless it is treated promptly.
Early detection and treatment of eye conditions are key to the optimal preservation of sight.
Schedule an assessment should you experience any eye discomfort or vision problems.
What causes retinal detachment?
A clear gel called the vitreous humour fills the back of the eye, just in front of the retina. As one ages, the vitreous may pull away from its attachment to the retina. Usually, when this separation occurs, no problems arise. Occasionally, this separation can cause a tear in the retina. Fluid may pass through this retinal tear, causing the retina to be lifted off the wall of the eye, and this constitutes a retinal detachment.
The following conditions put a person at greater risk of retinal detachment:
- Short-sightedness or myopia
- Previous cataract surgery
- Eye injury
- Retinal detachment in the other eye
- Family history of retinal detachment
What are the symptoms / warning symptoms of retinal detachment?
The following may indicate the presence of retinal detachment (but do not always mean a retinal detachment is present)
- Flashes
- Sudden onset or increase in floaters
- A shadow in the periphery of your field of vision
- A gray curtain moving across your field of vision
If you experience any of these symptoms, it is best that you consult an eye doctor immediately.
What happens during the diagnosis of retinal detachment?
When your eye doctor examines your eyes, eye drops to dilate (enlarge) your pupils will first be instilled. This pupil dilation is necessary for the doctor to have a good, all round view of the vitreous cavity and retina inside your eye. This is important to diagnose the retinal detachment and to determine the exact location of the detachment and associated retinal tears.
All about retinal detachment surgery
How are retinal tears and retinal detachment treated?
How are retinal tears and retinal detachment treated?
- Retinal tears without retinal detachment
Retinal tears are usually treated with laser surgery which seals the retina around the tear to the back wall of the eye. This prevents a retinal detachment from developing.
- Retinal detachment
Retinal detachments are treated surgically to return the retina to its proper position. The decision on the type of surgery and anaesthesia (general or local) depends on the characteristics of the detachment, and the expertise of your surgeon.
In cases associated with a tear in the retina, the tear has to be sealed through the use of laser (endolaser) or cryotherapy (freezing).
Types of retinal detachment surgery:
- Scleral Buckle
This involves placing a flexible band, like a belt buckle (the scleral buckle) around the eye to counteract the forces pulling the retina out of place. The surgeon has to also drain the fluid under the detached retina (subretinal fluid drainage), to allow the retina to settle back into its normal position against the back wall of the eye.
- Vitrectomy
The vitreous humour or gel, is removed from the eye by a sophisticated cutting instrument, the vitrector, and the space is temporarily filled with gas or silicone oil.
Vitrectomy is sometimes combined with scleral buckling.
- Pneuumatic Retinopexy
A gas bubble is injected into the vitreous cavity of the eye to push the retina tear against the back wall of the eye for it to reattach.
What precautions must I take if a gas bubble is left in my eye after the surgery?
Immediately after the surgery, your surgeon will ask you to maintain a certain head posture for a few days. The gas bubble will gradually disappear over time.
You will be instructed not to fly in an aeroplane or travel at high altitude until the gas bubble disappears. A rapid increase in altitude can cause the gas to expand in your eye, and this can cause a dangerous rise in eye pressure.
What are the risks of retinal detachment surgery?
Some of the risks include a rise in pressure in the eye, cataract, infection, bleeding or re-detachment. Sometimes more than one surgery is required to fully attach the retina.
Recovery After Retinal Detachment Surgery
Vision usually takes months to improve, and in some cases, may not return fully to normal. Generally, the more severe the detachment, and the later the patient presents to the doctor, the less likely the operation will be successful. It is therefore very important for you to seek treatment early once there is a suspicion of a retinal detachment.
